Share this
saliva microsampling: lessons from COVID-19
by Neoteryx Microsampling on Jun 21, 2021 9:00:00 AM
The COVID-19 pandemic provided researchers with a unique opportunity to explore several different types of bio-fluid collection and testing. The crisis helped experts understand which methods work best in different settings, scenarios and studies.
 Nasopharyngeal (NP) swabs for RT-PCR testing served as the first-line method for detecting active infection with COVID-19 during the coronavirus pandemic. This method is effective and relatively easy to administer, but it is also very uncomfortable and difficult to conduct on children and some patients with disabilities. The NP swab method also has produced frequent false-negative results and has led to some complications.
Nasopharyngeal (NP) swabs for RT-PCR testing served as the first-line method for detecting active infection with COVID-19 during the coronavirus pandemic. This method is effective and relatively easy to administer, but it is also very uncomfortable and difficult to conduct on children and some patients with disabilities. The NP swab method also has produced frequent false-negative results and has led to some complications.
 During the Coronavirus Pandemic, researchers also used blood samples for serology studies to determine if people who had recovered from COVID-19 had developed antibodies against the SARS-CoV-2 virus. Due to widespread lockdowns and safety concerns during the coronavirus pandemic, many researchers obtained finger-stick blood samples remotely using Mitra® devices for microsampling studies. Blood testing was the dominant method used to examine both natural and vaccine-induced immunity response to SARS-CoV-2.
During the Coronavirus Pandemic, researchers also used blood samples for serology studies to determine if people who had recovered from COVID-19 had developed antibodies against the SARS-CoV-2 virus. Due to widespread lockdowns and safety concerns during the coronavirus pandemic, many researchers obtained finger-stick blood samples remotely using Mitra® devices for microsampling studies. Blood testing was the dominant method used to examine both natural and vaccine-induced immunity response to SARS-CoV-2.
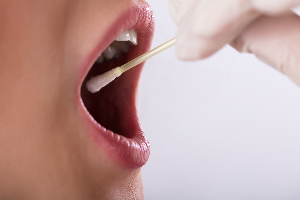 Researchers also used saliva testing during the pandemic. The ease of use and results of some SARS-CoV-2 saliva sampling studies generated significant interest in this type of bio-fluid testing. Saliva testing is certainly more comfortable and convenient for study participants.
Researchers also used saliva testing during the pandemic. The ease of use and results of some SARS-CoV-2 saliva sampling studies generated significant interest in this type of bio-fluid testing. Saliva testing is certainly more comfortable and convenient for study participants.
In a study by researchers at Yale School of Medicine, saliva was found to better predict the severity of COVID-19 disease progression in individuals. This was because the saliva samples collected for this study provided better estimates of viral load compared to other bio-fluid samples.
A New Frontier for Bio-fluid Testing
Saliva testing in research has traditionally been challenging due to a lack of sufficiently powerful lab equipment. Analyzing the full spectrum of biomarkers present in saliva requires sensitivity between 1,000-10,000 times higher than what older equipment is typically capable of. Newer equipment is much more powerful, and now that these newer models have started to become more widely available in laboratories, saliva testing also has become more viable.
Researchers are still exploring what kinds of information they can derive from saliva sampling and testing, but early applications suggest it can be used to uncover at least as much biological information as most other bio-fluid testing. It may also be useful in detecting conditions that are not currently screened with bio-fluids, including concussions.
How Saliva Sampling Works
Because researchers can extract all the biological information they need from very small saliva samples, saliva microsampling can work well in many studies. With microsampling, the sample collection process can be conducted remotely or in-person using some microsampling devices.
 Some researchers have sent these devices to study participants at home in Mitra collection kits, which contain all the supplies needed for sample collection. This is a simple user-centric process that allows trial subjects to self-collect samples at any time and in any setting they choose.
Some researchers have sent these devices to study participants at home in Mitra collection kits, which contain all the supplies needed for sample collection. This is a simple user-centric process that allows trial subjects to self-collect samples at any time and in any setting they choose.
In clinical trials that offer a remote option for participation, the trial subject typically receives a specimen collection kit in the mail and unpacks the collection devices and other supplies for sampling in the comfort of their own home.
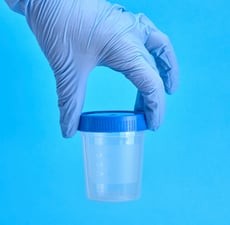 For saliva collection, a sputum cup can be enclosed in the kit. Trial subjects must spit into the cup several times to amass a small pool of saliva. The subject then holds the tip of each of their two Mitra devices in the saliva for about 2 seconds.
For saliva collection, a sputum cup can be enclosed in the kit. Trial subjects must spit into the cup several times to amass a small pool of saliva. The subject then holds the tip of each of their two Mitra devices in the saliva for about 2 seconds.
Once the microsampling device tips are filled with the saliva specimens, the devices are closed inside their protective casing. The devices are placed into a specimen pouch and a prepaid envelope from the kit and mailed back to the lab for analysis.
The entire sample collection process takes just a few minutes from start to finish and can be performed by anyone following the simple instructions provided. This sampling method greatly expands the possible applications for saliva testing in a range of research studies.
A custom version of at-home kits may allow for the possibility of providing study participants with supplies & devices for collecting different types of samples (e.g., saliva, blood, urine).
Future Applications of Saliva Sampling
Saliva sampling may be used for new applications in the future, which may provide new insights. For example, there are many diseases that don’t shed biomarkers in blood but may shed them in saliva.
Using saliva sampling could help researchers and clinicians test for and treat illnesses that are currently difficult to detect using blood testing alone. Saliva testing also has potential in toxicology applications and may present an attractive alternative to messy drug and alcohol tests, such as urine testing.
There are also situations in which saliva microsampling may offer unique advantages over other methods. For instance, saliva microsampling can be used to test for HIV with nearly the same level of precision as blood testing, while providing a more comfortable user experience. Saliva sampling can also minimize the risk of accidental disease transmission.
Exploring Saliva’s Potential
The full range of possibilities for saliva sampling remains untapped, but after the promise it showed during the COVID-19 pandemic, it merits further investigation. The non-invasive comfort and convenience of saliva microsampling vs. more invasive specimen sampling suggests that more sampling applications of this bio-fluid are worth implementing on a wider scale.

Image Credits: Trajan, iStock, Shutterstock
Share this
- Microsampling (206)
- Research, Remote Research (119)
- Venipuncture Alternative (105)
- Clinical Trials, Clinical Research (83)
- Mitra® Device (73)
- Therapeutic Drug Monitoring, TDM (51)
- Dried Blood Spot, DBS (39)
- Biomonitoring, Health, Wellness (30)
- Infectious Disease, Vaccines, COVID-19 (24)
- Blood Microsampling, Serology (23)
- Omics, Multi-Omics (21)
- Decentralized Clinical Trial (DCT) (20)
- Specimen Collection (18)
- Toxicology, Doping, Drug/Alcohol Monitoring, PEth (17)
- Skin Microsampling, Microbiopsy (14)
- hemaPEN® Device (13)
- Preclinical Research, Animal Studies (12)
- Pharmaceuticals, Drug Development (9)
- Harpera Device (7)
- Industry News, Microsampling News (5)
- Antibodies, MAbs (3)
- Company Press Release, Product Press Release (3)
- Environmental Toxins, Exposures (1)
- July 2025 (1)
- May 2025 (1)
- April 2025 (2)
- December 2024 (2)
- November 2024 (1)
- October 2024 (3)
- September 2024 (1)
- June 2024 (1)
- May 2024 (1)
- April 2024 (4)
- March 2024 (1)
- February 2024 (2)
- January 2024 (4)
- December 2023 (3)
- November 2023 (3)
- October 2023 (3)
- September 2023 (3)
- July 2023 (3)
- June 2023 (2)
- April 2023 (2)
- March 2023 (2)
- February 2023 (2)
- January 2023 (3)
- December 2022 (2)
- November 2022 (3)
- October 2022 (4)
- September 2022 (3)
- August 2022 (5)
- July 2022 (2)
- June 2022 (2)
- May 2022 (4)
- April 2022 (3)
- March 2022 (3)
- February 2022 (4)
- January 2022 (5)
- December 2021 (3)
- November 2021 (5)
- October 2021 (3)
- September 2021 (3)
- August 2021 (4)
- July 2021 (4)
- June 2021 (4)
- May 2021 (4)
- April 2021 (3)
- March 2021 (5)
- February 2021 (4)
- January 2021 (4)
- December 2020 (3)
- November 2020 (5)
- October 2020 (4)
- September 2020 (3)
- August 2020 (3)
- July 2020 (6)
- June 2020 (4)
- May 2020 (4)
- April 2020 (3)
- March 2020 (6)
- February 2020 (3)
- January 2020 (4)
- December 2019 (5)
- November 2019 (4)
- October 2019 (2)
- September 2019 (4)
- August 2019 (4)
- July 2019 (3)
- June 2019 (7)
- May 2019 (6)
- April 2019 (5)
- March 2019 (6)
- February 2019 (5)
- January 2019 (8)
- December 2018 (3)
- November 2018 (4)
- October 2018 (7)
- September 2018 (6)
- August 2018 (5)
- July 2018 (8)
- June 2018 (6)
- May 2018 (5)
- April 2018 (6)
- March 2018 (4)
- February 2018 (6)
- January 2018 (4)
- December 2017 (2)
- November 2017 (3)
- October 2017 (2)
- September 2017 (4)
- August 2017 (2)
- July 2017 (4)
- June 2017 (5)
- May 2017 (6)
- April 2017 (6)
- March 2017 (5)
- February 2017 (4)
- January 2017 (1)
- July 2016 (3)
- May 2016 (1)
- April 2016 (2)


No Comments Yet
Let us know what you think