Share this
by Neoteryx Microsampling on Jan 17, 2018 5:03:00 AM
Practical strategies to enhance patient empowerment
- Provide reasonable choices whenever feasible, such as options for medication timing, reminder methods, and follow-up formats.
- Ask about barriers early (“What might get in the way of taking this consistently?”).
- When clinically appropriate, implement patient-centric sampling options to minimize obstacles and enhance engagement. (link.springer.com)
- Consider integrating digital technologies, wearable devices, and remote specimen collection to support self-monitoring and decrease dependence on frequent in-clinic visits.
3) Economic Constraint Reduction
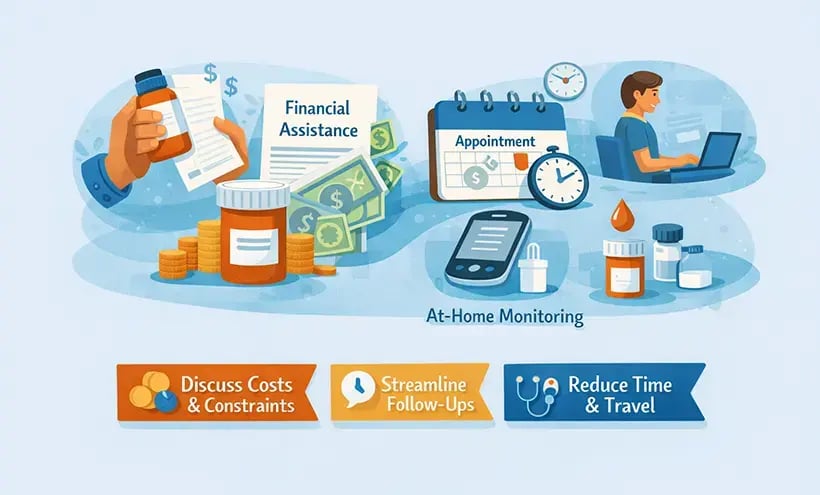
Although many patients intend to adhere to prescribed medication regimens, financial constraints can significantly impede their ability to do so. Common challenges include:
- Cost of medicine
- Arranging work around potential side effects
- Missing work to attend medication reviews
Facilitating access to financial assistance, offering appointments at convenient times, and enabling at-home monitoring through technological advancements, such as remote blood collection, can substantially improve medication adherence.
Additionally, self-monitoring and remote monitoring approaches reduce the frequency of clinic visits, allowing patients to maintain employment while remaining engaged in their care. Practical strategies to address economic constraints
- Proactively discuss affordability and work constraints (patients may not raise this on their own).
- Streamline follow-up procedures and minimize unnecessary in-person visits when clinically appropriate.
- Adopt monitoring approaches that decrease the time, travel, and appointment burden for patients. (link.analytica-chimica-acta)
4) Patient–Physician Relationship Building

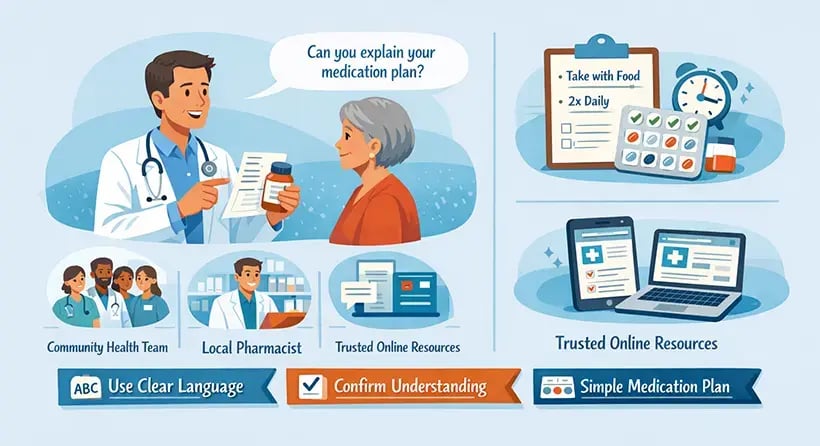
Trust, respect, and understanding, established by considering patients’ religious and cultural beliefs and attitudes, are essential for promoting medication adherence.
Physicians should explain the composition of medications and, when necessary, offer alternative therapies that align with the patient's beliefs.
Patients who trust their physicians are more likely to adhere to prescribed medication regimens. Practical strategies to enhance patient–physician relationships
- Normalize adherence challenges to encourage honesty (patients may fear judgment).
- Encourage early discussions regarding patients' beliefs, concerns, and preferences.
- Ensure that follow-up interactions are supportive and non-punitive.
5) Adverse-Effects Mitigation

Adverse effects of medication are a significant concern for many patients. Encountering information about potential side effects solely through medication package inserts can be overwhelming and distressing.
Physicians can significantly improve medication adherence by explaining potential adverse effects, their likelihood, and appropriate actions to take if they occur. Practical strategies to mitigate adverse effects
- Explain what is common vs. rare, and what to do if symptoms occur.
- Establish clear criteria for when patients should contact the clinic or seek urgent care.
- Emphasize that managing side effects is an integral component of the treatment plan, rather than an indication of failure.
Closing the gap — development of an analytical methodology using volumetric absorptive microsampling of finger prick blood followed by LC-HRMS/MS for adherence monitoring of antihypertensive drugs ( Research Paper. Published: Volume 415, pages 167–177, (2023) https://link.springer.com/article/10.1007/s00216-022-04394-9
A Comprehensive, Patient-Centered Approach
No single approach is sufficient in isolation. To substantially improve medication adherence across patient populations, these strategies should be integrated into a comprehensive, patient-centered framework that combines clear education, shared decision-making, relationship-centered care, side-effect management, and, when appropriate, self-monitoring options such as digital tools, wearable devices, and remote specimen collection.

Further supporting publications (patient-centric microsampling for adherence monitoring)
- VAMS method in finger-prick blood applicable for adherence monitoring of antipsychotics (published Jan 30, 2021). (link.springer.com)
- VAMS finger-prick blood methodology for adherence monitoring of antihypertensive drugs; the article notes VAMS suitability and comparable adherence classification to plasma in their proof-of-concept. (link.springer.com)





Comments (1)